 A new study on rheumatoid arthritis entitled “Maintenance of remission following 2 years of standard treatment then dose reduction with abatacept in patients with early rheumatoid arthritis and poor prognosis” was published in the Annals of the Rheumatic Diseases by Prof. Rene Westhovens from the Department of Rheumatology, Leuven, Belgium, and colleagues.
A new study on rheumatoid arthritis entitled “Maintenance of remission following 2 years of standard treatment then dose reduction with abatacept in patients with early rheumatoid arthritis and poor prognosis” was published in the Annals of the Rheumatic Diseases by Prof. Rene Westhovens from the Department of Rheumatology, Leuven, Belgium, and colleagues.
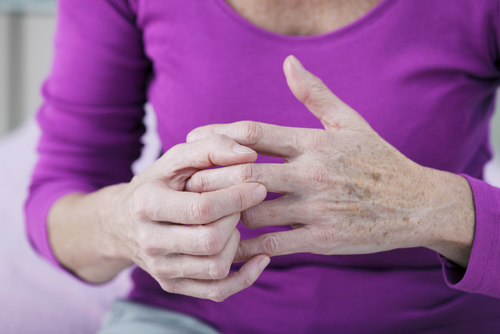
Rheumatoid arthritis (RA) is a common autoimmune, inflammatory disease associated with progressively debilitating, systemic complications, socioeconomic costs and early death. The etiology of rheumatoid arthritis is unknown. Advances in rheumatoid arthritis have led to the development of new therapeutic medicines that have improved disease outcome. The actual strategy of treatment is to start with an aggressive therapy shortly after diagnosis, with the use of disease-modifying antirheumatic drugs (DMARDs) in combinations, biologic therapies, and an escalation of therapy based on disease assessment activity, with the aim of clinical remission.
Normally, the majority of clinicians begin treatment by prescribing methotrexate, but only 30% of patients will have low disease activity. In these cases, the use of biological therapies and various combinations of conventional DMARDs are more successful than placebo when added to methotrexate. However, normally, clinicians prefer to prescribe tumor necrosis factor (TNF) inhibitors together with methotrexate, which are much more expensive than conventional DMARDs. The main goal of RA treatment is to achieve drug-free remission.
The research team decided to perform a substudy of the AGREE (Abatacept trial to Gauge Remission and joint damage progression in methotrexate-naive patients with Early Erosive rheumatoid arthritis) trial over 1-year, as a multinational, randomised, double-blind study to assess the effect of lowering the dose of intravenous abatacept from the approved dose of 10 mg/kg to 5 mg/kg per month on disease activity, in patients with early RA with poor prognosis that achieved a disease activity score (DAS) of 28, and erythrocyte sedimentation rate (ESR) lower than 2.6 after 2 years of standard treatment. The primary outcome was time to disease relapse consisting on the use of extra DMARS, ≥2 courses high-dose steroids, a return to open-label abatacept 10 mg/kg, or DAS28 (C reactive protein) ≥3.2 at two consecutive visits).
The research team concluded in this trial that the use of a lower dose of abatacept could be a possibility for the treatment of patients with early RA, and poor prognosis that reached DAS28, with (ESR) lower than 2.6 after 1 year of monotherapy with abatacept (∼10 mg/kg).