 During the American College of Rheumatology annual meeting held in Boston this past November, several research projects related to rheumatoid arthritis were presented. Among them, a novel blood test that could lead to improvements in prescribing effective medication for RA patients.
During the American College of Rheumatology annual meeting held in Boston this past November, several research projects related to rheumatoid arthritis were presented. Among them, a novel blood test that could lead to improvements in prescribing effective medication for RA patients.
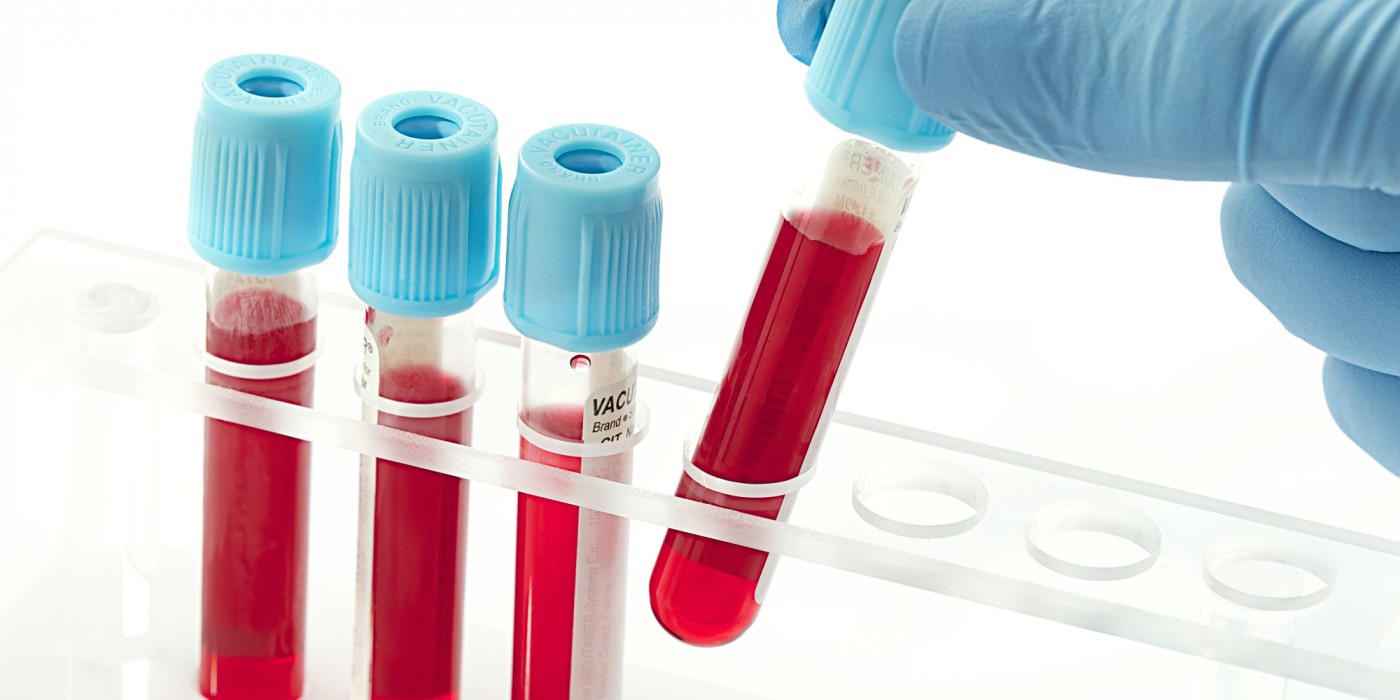
A new study on rheumatoid arthritis led by the group of Timothy Niewold, M.D., a rheumatologist at Mayo Clinic in Rochester, Minnesota, identified that type 1 interferon, a cytokine made by the immune cells in the blood could be used as a potential marker to stratify the treatment response of patients with rheumatoid arthritis to standard biological agents used for RA therapy, or if other drugs should be given. For this, the researchers took blood from patients with rheumatoid arthritis before treatment to measure type 1 interferon and then the patients were prescribed anti-inflammatory biologic drugs, inhibitors of tumor necrosis factor-alpha, a novel group of rheumatoid arthritis drugs. This protein can be measured in blood tests to help avoid trial and error with prescriptions, avoiding delays in the treatment, unnecessary advert events and expenditure by the patients.
“We are trying to personalize therapy for rheumatoid arthritis. One of the main problems rheumatologists have had is that it’s hard to choose the right drug for the right person,” said Dr. Timothy Niewold, in the press release.
“Each new drug works for some people and not others. It’s not trivial, because the disease causes damage in the joints and if it takes a year or two to find the right treatment, then damage can accrue,” said Dr. Niewold. “In the study, we looked at markers in the immune system that might help.”
The first standard procedure for rheumatoid arthritis therapy is Methotrexate, an antimetabolite and antifolate drug. If this medication does not work, clinicians normally give the second option therapy, biologics. The biologics have many advert effects like risk of infection and, prior to this therapy, patients had to be screened for tuberculosis.
Dr. Niewold stated that the treatment of rheumatoid arthritis should be prompt since it’s crucial to prevent the damage that the disease causes directly, but also to reduce the probability of other severe diseases, such as cardiac disease. Rheumatoid arthritis patients have twice as much risk of developing cardiac conditions than healthy patients, and according to previous research by Mayo Clinic researchers, this risk is associated with the severity of the rheumatoid arthritis. Notably, patients where methotrexate therapy had no effect develop more severe rheumatoid arthritis.
According to Dr. Niewold, there is still a long way before type 1 interferon can be used as marker and become a standard procedure. Dr. Niewold added that a larger clinical trial with several institutions is currently being prepared, and future studies will be useful to evaluate if type 1 interferon could be used as marker for other diseases treated with biologics, such as psoriatic arthritis, psoriasis and inflammatory bowel disease, he says.
In another study presented at the American College of Rheumatology meeting, researchers found that patients with rheumatoid arthritis and their physicians have different conceptions of pain, leading to a gap in understanding between the two. Researchers found that patients describe pain using words with emotional expressions, while physicians likely explain pain using sensory words such as “sharp, aching or throbbing”. Additional research is needed to help clinicians develop new methods to better alleviate pain.
Patients with rheumatoid arthritis have flare-ups that increase the risk of developing cardiac disease. “Every time joints flare up, it’s a knock against their hearts,” said co-author Eric Matteson, M.D., rheumatology chair at Mayo Clinic in Rochester, in the press release. “Patients should keep track of their flare-ups and call their physician when they have a flare.”
The researchers said that patients with psoriatic arthritis are also at higher risk of cardiac disease. Thus, prevention, detection and treatment of cardiac disease are very important for these patients.
The study of type 1 interferon was funded by The Rheumatology Research Foundation and National Institutes of Health.